Alternative names for carcinoid tumour
Neuroendocrine tumour; neuroendocrine tumor; NET; neuroendocrine carcinoma; carcinoid tumor
What is a carcinoid tumour?
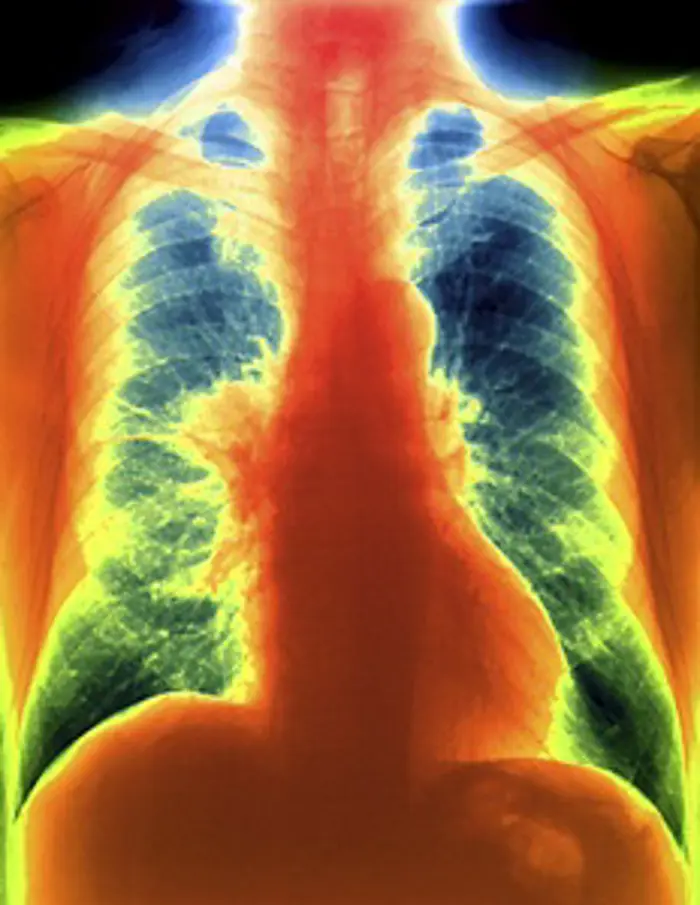
Coloured frontal chest X-ray of a patient with a carcinoid tumour (red, centre left) in their right lung.
Carcinoid tumours are part of a group of tumours called neuroendocrine tumours. These tumours are made from specialised cells that produce and release hormones. These hormones are released into the bloodstream and can have effects on other organs.
Neuroendocrine tumours can appear in a number of places, including all parts of the digestive system (oesophagus, stomach, small bowel, appendix, large bowel, rectum, pancreas and liver), the respiratory system (bronchi and lungs) and, less commonly, the reproductive system (ovaries and testes).
Carcinoid tumours tend to grow and spread much more slowly than other cancers of the digestive system.
What causes carcinoid tumours?
Carcinoid tumours grow from neuroendocrine cells. The trigger for this process is not known, but it is thought that most occur by chance.
In some cases, a genetic link may be the cause. Multiple endocrine neoplasia type 1 is a genetic disorder that increases the risk of neuroendocrine tumours, including carcinoids, while digestive system conditions (such as pernicious anaemia and atrophic gastritis) can increase the risk of carcinoid tumours of the digestive tract.
What are the signs and symptoms of a carcinoid tumour?
Carcinoid tumours may be discovered by chance and may produce very few symptoms. However, they do sometimes cause signs and symptoms which may result from both the tumour itself and any hormones released into the bloodstream:
- Signs and symptoms caused by the growing tumour
These effects depend on the location of the tumour. For example, a carcinoid tumour in the lung might cause a cough, including coughing up blood. A carcinoid tumour in the gut may result in abdominal pain, feeling sick, and bleeding from the bottom.
- Signs and symptoms caused by secretion of hormones
Carcinoid syndrome is the collection of signs and symptoms relating to the release of hormones, such as serotonin, from a carcinoid tumour into the bloodstream. This is more common when the tumour cells have spread to the liver. The signs and symptoms can include flushing of the skin (especially brought on by food and alcohol), diarrhoea, fast heart rate, and wheezing. This can also rarely lead to a carcinoid crisis, which is a serious condition involving changes in blood pressure, breathlessness, and severe flushing.
- Signs and symptoms caused by long-term raised hormone levels
Some of the hormones released by carcinoid tumours can cause the development of fibrous tissue in various organs. This may lead to heart valve problems, breathlessness and swollen ankles. The fibrous tissue surrounding intestinal carcinoid tumours can lead to formation of adhesions and obstruction of the intestine. Production of large amounts of these hormones can also use up a large part of the body’s vitamin B stores, resulting in nerve damage, particularly in the feet and lower legs.
How common are carcinoid tumours?
Carcinoid tumours are relatively rare. Around 4,000 people in the UK are diagnosed with neuroendocrine tumours each year, of which a proportion are carcinoid tumours. As survival rates with these tumours are generally good, the number of people living with these conditions is relatively higher.
How is a carcinoid tumour diagnosed?
Carcinoid tumours may be detected by chance, for example on an abdominal scan or chest X-ray, or during surgery performed on the gut for another reason.
In a patient with symptoms such as diarrhoea and flushing suggestive of carcinoid syndrome, a 24 hour urine sample is collected to measure the levels of 5-hydroxyindolacetic acid, which is produced from breakdown of a particular chemical (tryptophan). This test can be performed as an outpatient. It is necessary to stick to a special diet during the collection period, avoiding foods such as bananas, chocolate, walnuts and avocado, as these foods can also cause higher levels of 5-hydroxyindolacetic acid in the urine.
Chromogranin A levels in blood is a useful marker to assess for presence of carcinoid tumour as well as providing information on disease load. Utility of chromogranin A levels include measurement after surgery to assess if there is any residual carcinoid tumour remaining, and monitoring for disease progression while the patient is being treated with medications.
Carcinoid tumours often have a particular appearance on computerised tomography (CT) scans. Looking at a sample of tumour tissue under the microscope (histology) will usually provide a definitive diagnosis. CT scans are also helpful in demonstrating the disease extent and spread. Specialist nuclear medicine scans such as octreotide or MIBG scans may be used after the tumour is diagnosed. These are helpful to assess the tumour spread and extent, and for planning future therapy. The doctor may also arrange some tests to evaluate if any damage has been caused to the heart valve by arranging an echocardiogram.
How is a carcinoid tumour treated?
It is recommended that multidisciplinary teams at referral centres provide guidance on the management of the patient. The main aim should be to keep the patient disease and symptom-free for as long as possible and to maintain a good quality of life.
The definitive treatment for a carcinoid tumour is by surgical removal of the tumour. However, surgical cure may not be possible if the tumour has spread to other organs, or is too big to remove. In this situation, other treatment options which may be effective can be used:
- Injections of somatostatin analogues (such as octreotide or lanreotide), an equivalent of a naturally produced hormone called somatostatin, which can reduce hormone production and even possibly slow down the growth and spread of the tumour.
- Chemotherapy, which are medicines that kill fast-growing cells and reduce the size of the tumour.
- Localised tumour directed therapy, such as radiotherapy (a treatment where radiation is used to kill tumour cells), radiofrequency ablation (a procedure that uses a heated probe to kill tumour cells, and hepatic artery embolisation (a procedure to block the blood supply to the tumour in the liver).
- Targeted therapy, which is a type of treatment that target certain genes or proteins to kill tumour cells such as sunitinib, everolimus, and interferon
- Peptide receptor radionuclide therapy (PRRT), which is a type of internal targeted radiotherapy that uses a radioactive substance attached to a peptide (small protein) that targets the tumour cells.
What are the longer-term implications of a carcinoid tumour?
As with all cancers, the main implication of carcinoid tumours is their continued growth and spread, together with the signs and symptoms of relating to release of hormones. Tumour growth usually occurs fairly slowly compared with other cancers. It is possible to live for a long time and with a good quality of life with a carcinoid tumour.
Sometimes patients with carcinoid syndrome may develop a carcinoid crisis that can be triggered by certain drugs or anaesthetic. Complications can also develop in other organs such as the heart and intestines relating to long-term raised hormone levels, which will require specialist management.

