Hypercortisolism; Cushing syndrome
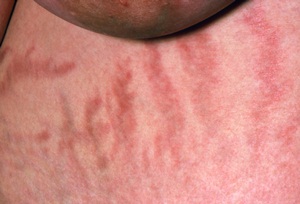
Photo of stretch marks on a woman suffering from Cushing's syndrome.
Cushing’s syndrome is a disorder that occurs when the body is exposed to an excess of the hormone cortisol or similar synthetic versions. The hormone cortisol belongs to a group of hormones called steroids and regulates various biological pathways including stress. Cushing’s syndrome can occur either because:
Cortisol is a steroid hormone produced by the adrenal glands, which sit on top of the kidneys. The adrenal glands are stimulated by a pituitary hormone called adrenocorticotropic hormone (ACTH) to release cortisol into the bloodstream.
There are a number of causes of Cushing’s syndrome:
Cushing’s syndrome is characterised by the following signs and symptoms:
The most common form of Cushing’s syndrome is the exogenous form, i.e. due to the patient taking an excess of steroid medication. Endogenous Cushing’s syndrome is rarer and is estimated to affect 1 in 500,000 adults per year. Of these, 85% have pituitary-dependent Cushing’s syndrome, 10% have adrenal Cushing’s and 5% have ectopic adrenocorticotropic hormone production (from a non-pituitary tumour).
Cushing’s syndrome is not usually inherited, but in very rare cases can run in families.
Patients with suspected Cushing’s Syndrome have diagnostic screening tests to confirm whether it is present. The clinical suspicion of Cushing’s syndrome is more accurate than any test. Before embarking on any tests, it is important to check if steroids are present in current medication the patient is taking, to rule out exogenous Cushing’s syndrome. Steroids can be found in prescription medications such as tablets, creams, ointments, inhalers, drops or sprays. Occasionally, steroids may be found as a contaminant in certain herbal preparations.
The initial screening tests are the overnight dexamethasone suppression test, the low dose dexamethasone suppression test or 24h urine collection for cortisol levels, and more recently late night salivary cortisol levels. In the suppression tests, a synthetic steroid called dexamethasone is taken late at night followed by a blood test for cortisol at 9 a.m. the next morning. In patients without Cushing’s syndrome, cortisol levels are suppressed to low levels but in patients with Cushing’s syndrome cortisol levels will remain un-suppressed. After confirmation of Cushing’s syndrome, the causes of the syndrome are differentiated by further tests.
Further blood tests include the measurement of ACTH levels (low in adrenal tumours) and the corticotropin-releasing hormone (CRH) and other dynamic tests may distinguish pituitary disease from ectopic ACTH. Specialised computerised tomography (CT) scans of the adrenal glands or magnetic resonance imaging (MRI) scans of the pituitary may help determine the source of Cushing’s although false negative or positive results are possible so need an expert endocrine opinion.
Inferior petrosal sinus sampling (IPSS) may be carried out to determine whether the source of ACTH production is within the pituitary gland and to distinguish this from ectopic ACTH. This involves placing thin plastic tubes, under local anaesthetic, into a vein in the groin area (the area of the hip between the stomach and the thigh). These are threaded into the blood vessels next to the pituitary gland with the aid of an X-ray machine and are used to take blood samples, after an intravenous injection of CRH. The blood samples will help distinguish Cushing’s disease from ectopic ACTH production.
A bone mineral density test may also be carried out to examine if the patient has reduced bone density and to determine the risk of developing osteoporosis (weakened and thinner bones) as well as a screening test for diabetes mellitus.
It may take some time before investigations are complete and Cushing’s syndrome is diagnosed.
Exogenous Cushing’s syndrome is treated by gradually reducing the steroid drug dose under medical supervision, whenever possible. This must be done in conjunction with the specialist who prescribed the steroid drug. In some serious conditions, the steroids cannot be stopped. For some conditions, there are alternative drugs to steroids, but these might have their own side-effects. It is very important that the patient does not stop taking any steroid medication without discussing it with their doctor.
Depending on the cause, endogenous Cushing’s syndrome is treated by surgery, medication, or radiotherapy. Patients should be treated in a specialist centre with dedicated endocrinologists and surgeons working in a multidisciplinary team. The main goals of treatment are to bring cortisol levels back to normal, to reverse signs and symptoms and to maintain control in the long term.
For Cushing’s disease patients who have received a surgery, some may experience loss of sensation of smell temporarily, which usually returns to normal after a few weeks or months. Some may feel thirsty and urinate more often, a condition known as Diabetes Insipidus, which is usually temporary but can be permanent occasionally. Such condition is usually improved after prescription of a drug called desmopressin.
In addition, some may feel weaker in strength and experience mood changes due to a temporary suppression in the body’s cortisol production. To relieve these effects, it is often necessary for the patient to take hydrocortisone tablets to replace the cortisol hormone. Patients would become very unwell if this treatment is stopped without ensuring that production of cortisol has returned. Hydrocortisone tablets are taken two to three times a day until normal pituitary and adrenal function is restored. This could be for several months or patients may need to continue taking hydrocortisone for life.
If pituitary surgery or radiotherapy is carried out, the patient may develop deficiencies of other pituitary hormones (hypopituitarism), which may need replacement tablets. It may be necessary for the patient to take tablets for life to replace these essential pituitary hormones.
Tablets taken to reduce cortisol levels can have side-effects on the liver and kidneys, so regular blood tests are carried out to make sure the patient is on the correct dose and that there are no serious problems.
Following successful treatment of Cushing’s syndrome, it may take between several weeks and a couple of years for the changes due to excessive cortisol production to return to normal and for the symptoms to disappear. Muscle and bone strength will improve, but some patients, particularly post-menopausal women, may need treatment for osteoporosis. Blood pressure and blood sugar should be closely monitored.
Patients may need to take hydrocortisone replacement tablets for life. Higher doses of hydrocortisone must be supplied for medical emergencies as the body is unable to make its own cortisol in response to stressful situations. Patients should also carry an intramuscular hydrocortisone injection in case of emergency, a steroid card, and wear Medic-Alert jewellery.
It is important to recognise that even after treatment for Cushing’s syndrome, some patients do not regain their original quality of life, or it can take many months or years. The amount of investigations, treatment and follow-up means that genuine diagnosis of Cushing’s is very time consuming for the patient and their relatives.
Pituitary Foundation may be able to provide advice and support to patients and their families dealing with Cushing's syndrome.
Last reviewed: Nov 2020