Klinefelter’s syndrome; Klinefelter syndrome; 47 XXY syndrome; XXY syndrome; XXY trisomy
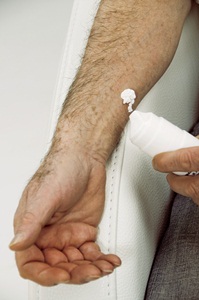
Man applying a skin cream containing testosterone used to replace this sex hormone in men who have lost their sex drive, or had their testes removed due to cancer or other diseases.
Klinefelter syndrome is a genetic disorder whereby a boy is born with one (or more) extra X chromosomes. Chromosomes carry our genetic information. Humans have 23 pairs of chromosomes (total 46 chromosomes), half of which are inherited from each parent. One pair is the sex chromosomes, which determine the sex – boys usually have an X and a Y chromosome (XY), whereas girls have two X chromosomes (XX). So rather than having the usual 46 chromosomes, they may have 47 chromosomes due to the extra X chromosome, and thus be described as 47 XXY.
The extra one (or more) X chromosomes in Klinefelter syndrome may cause a number of features including tall stature, small testes, less pubic and facial hair, reduced fertility, development of breast tissue (gynaecomastia) and sometimes problems with language and social interactions.
There is, however, a wide variation in the clinical presentation amongst individuals with Klinefelter syndrome, and many cases remain undiagnosed.
Klinefelter syndrome is named after Dr Harry Klinefelter, who first described a collection of symptoms present in men with an extra X chromosome.
Klinefelter syndrome is caused by men having an extra one (or more) X chromosomes. This occurs as a result of a problem in the way cells divide either before or after conception. The usual 47 XXY pattern of Klinefelter’ syndrome accounts for around 80% of cases, however, there are also other variations. Sometimes, more than one extra X chromosome is present resulting in 48 or 49 chromosomes (48 XXXY or 49 XXXXY). Another variation is that not all cells in the affected individual have an extra X chromosome; this is known as mosaicism. The greater the number of cells containing an extra X chromosome, the more likely it is to lead to features of Klinefelter syndrome.
Not all individuals with this condition have the same symptoms or to the same extent; because of this variability in symptoms, many men can often remain undiagnosed. Symptoms depend on the proportion of cells in the body that contain an extra X chromosome (XXY), how much testosterone is being produced and the age at diagnosis.
From early school age, boys with Klinefelter syndrome tend to be taller (increased leg length) in part because testosterone (via conversion to oestrogen) normally stops the long bones from growing after puberty. This increase in height is maintained throughout life. Boys with Klinefelter syndrome may have reduced coordination compared with other boys.
Klinefelter syndrome may be diagnosed antenatally (i.e. before birth), if screening was undertaken for other conditions, or in infancy if the boy has a small penis or undescended testes (cryptorchidism). It may be diagnosed in a younger boy who presents with speech problems, or having difficulties with interaction with friends or at school. However, it is often not diagnosed until around puberty, when most boys with Klinefelter syndrome make less testosterone than unaffected boys. This can lead to a taller, less muscular appearance with less facial and body hair, a reduced sex drive (libido), difficulties maintaining erections (potency), and lower energy levels. Men with Klinefelter syndrome may develop breast enlargement (gynaecomastia) and thinning of the bones (osteoporosis). Characteristically, they have small, firm testes with a low or absent sperm count; almost all men who are 47 XXY will be infertile. However, most men with Klinefelter syndrome may have a normal sex life, especially when given appropriate treatment with testosterone replacement if this is reduced.
A significant proportion of men with Klinefelter syndrome have difficulty with language (problems with reading or learning to talk initially), or executive functions (problem solving, task switching, planning, etc.), not dissimilar to people with dyslexia. They may also have difficulty with social interactions throughout life, but particularly in childhood. The majority of men with Klinefelter syndrome lead an independent life, forming relationships and having a normal job and have a normal life span.
Klinefelter syndrome only affects men, and is one of the most common chromosome abnormalities in men. About 1 of every 650 live male births has an extra X chromosome, but many do not have any symptoms. Importantly, up to 3% of infertile men have Klinefelter syndrome and many cases go undiagnosed. It can often be diagnosed if a man is undergoing infertility testing.
Klinefelter syndrome is a genetic condition but it is not inherited from the parents. In the vast majority of boys, there are no other affected family members; it occurs sporadically (ie without a family history). The extra X chromosome can come from either the mother or the father. It is thought that older parents may be more likely to have a child with Klinefelter syndrome; this is probably because the risk of chromosomal abnormalities increases with age.
Where Klinefelter syndrome is suspected, blood tests will be carried out to assess levels of testosterone and gonadotrophins - LH (luteinising hormone) and FSH (follicle stimulating hormone). The blood tests characteristically show a low testosterone level, high sex hormone binding globulin (SHBG) and raised gonadotrophins (LH and FSH levels). The diagnosis of Klinefelter syndrome is confirmed by chromosomal analysis (karyotype), which is done using a blood test.
Karyotyping can also be performed during pregnancy by analysing the fluid surrounding the foetus (amniocentesis) or by obtaining placental tissue (chorionic villus sampling) in mothers of patients with Klinefelter syndrome to diagnose it before birth.
villus sampling). Both these procedures carry some risk and are performed as an inpatient.
The underlying chromosomal problem (XXY) cannot be changed, so the aim of treatment is to help with symptoms and prevent complications in the long-term, so early diagnosis is therefore beneficial. Treatment will differ among individuals depending on their age at diagnosis and the symptoms experienced.
Testosterone replacement therapy is important where levels are low, and may be required from the start of puberty. The dose is adjusted to maintain appropriate testosterone concentrations. Testosterone can be given in a number of ways but is usually given by gel, which is rubbed onto the skin every day, or by injection.
Testosterone replacement therapy helps to improve testosterone levels in order to aid muscle development, facial and body hair growth, and sex drive. It also helps to improve self-esteem, mood and maintain bone health. In addition, some men with Klinefelter syndrome may benefit from specialised fertility treatment to increase their chance of having children.
In individuals with Klinefelter syndrome who have developed breast enlargement, this sometimes becomes permanent. In these cases, surgery may be offered to reduce the amount of breast tissue.
Physical and occupational therapy may be helpful in affected boys with coordination and muscle problems.
Speech and behavioural therapy can help with difficulties with speech, developing language skills, confidence and academic performance. It is important that this support is offered as early as possible during childhood.
Testosterone replacement is generally well-tolerated, although care must be taken when treating some men such as those with prostate cancer. While on testosterone replacement therapy, a blood test is performed at least annually to check testosterone levels, blood count and also the health of the prostate (in men over 50 years of age). If testosterone replacement therapy is given by topical gel, this can sometimes lead to irritation of the skin at the site of application. If given by intramuscular injection, this can rarely cause pain and swelling at the site of the injection.
Less common side-effects include headache, mood change, nausea, jaundice, increased red blood cells, high blood pressure and fluid retention.
Adults with Klinefelter syndrome are more likely to have a number of health issues such as osteoporosis; obesity; varicose veins and leg ulcers; development of autoimmune conditions (diabetes mellitus, systemic lupus erythematosus and thyroid problems); chest conditions (bronchitis and emphysema); and there may be an increase in some cancers (breast cancer, germ cell tumours, non-Hodgkin’s lymphoma). Men with Klinefelter syndrome are also thought to be at an increased risk of developing chronic health problems such as cardiovascular, respiratory and gastrointestinal disease. Everyone with Klinefelter syndrome should therefore have regular check-ups during adult life, ideally in a specialist endocrinology clinic, both to monitor their general health and particularly to monitor testosterone replacement therapy.
Fertility problems are common in men with Klinefelter syndrome. However, more recent specialised fertility techniques, such as microsurgical testicular sperm extraction and intracytoplasmic sperm injection have helped some men with Klinefelter syndrome to father children. If patients have any concerns, they should discuss them with their doctor.
Klinefelter's Syndrome Association UK provide advice and support to patients and their families.
You can also find some further information and advice from the NHS here: https://www.nhs.uk/conditions/klinefelters-syndrome/
Last reviewed: Jul 2021