Stein-Leventhal syndrome; PCOS; polycystic ovarian syndrome
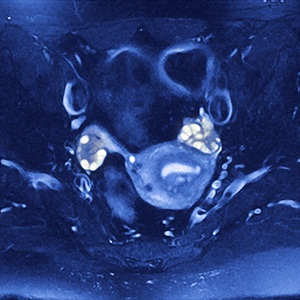
MRI scan of a female patient with polycystic ovary syndrome. Multiple cysts (white) have formed in the ovaries (centre left and right).
Polycystic ovary syndrome covers a variety of symptoms caused by problems with the balance of female reproductive hormones. Confusingly, women do not need to have cysts on their ovaries to be diagnosed with the condition. The signs and symptoms vary greatly among women.
Polycystic ovaries develop when the ovaries are stimulated to produce excessive amounts of male hormones (androgens), particularly testosterone, and it is this which is responsible for many of the symptoms experienced. The exact cause is not known, but it is thought that genetic and environmental factors play a part. Polycystic ovary syndrome tends to run in families and can in some circumstances be related to being overweight. There are also strong associations with diabetes and insulin resistance.
Polycystic ovary syndrome commonly causes problems relating to menstrual periods. They can become erratic, infrequent, or even stop altogether and this can cause reduced fertility. Other symptoms can include greasy skin or acne and there is often an increase in hair growth (hirsutism) in a male pattern (on the face, back and chest), which some women may find distressing. Symptoms get worse with weight gain.
Polycystic ovary syndrome is common in women of reproductive age. It is estimated to affect 5–10% of women in this group. However, more recent studies suggest that the number of women affected may be closer to 20%. Not all women will have symptoms.
Both genetic and environmental factors (such as weight gain) are thought to be important. There is often a family history of polycystic ovary syndrome or type 2 diabetes.
Polycystic ovary syndrome can be present at any age during the reproductive years and, because symptoms can vary considerably between individuals, it can take time to diagnose.
Women with polycystic ovary syndrome can have a variety of symptoms, including:
For a diagnosis of polycystic ovary syndrome to be made, at least two out of the three criteria listed above should be present, and other hormonal conditions giving rise to similar symptoms should be ruled out.
The diagnosis is made by taking a history of the symptoms, an examination and hormonal blood tests, which can be done as an outpatient. Women may or may not need to have an ultrasound scan of their ovaries.
Weight loss, although difficult, is usually recommended first line as this often helps reduce the symptoms of polycystic ovary syndrome. If becoming pregnant is not the most important objective, periods can usually be regulated with the oral contraceptive pill, sometimes containing a drug to block the actions of testosterone. Other medication used includes metformin (which is also often used in diabetes), spironolactone and cyproterone. These work in different ways to help overcome the hormonal imbalance, and the choice of treatment will depend in part on which symptoms are most problematic.
If a regular menstrual cycle is not desired, therapy for an irregular cycle is not necessarily required. Most experts consider that if a period occurs at least once every three months, the endometrium (lining of the uterus) is being shed often enough to prevent an increased risk of endometrial abnormalities or endometrial cancer. If periods occur less often or not at all, some form of progesterone replacement or the oral contraceptive pill may be recommended. Some women prefer a uterine progestogen device such as the Mirena coil or the progestin implant Implanon, which provides both contraception and endometrial protection for several years. An alternative is oral progestogen taken at intervals (e.g. every three months) to kick-start predictable menstrual bleeding.
If the woman has plans to get pregnant, and is not able to conceive naturally, then referral to a fertility service may be needed for treatments such as clomiphene to help them ovulate.
Metformin and spironolactone can cause stomach upset. Metformin may also cause dizziness, nausea and a metallic taste in the mouth.
Spironolactone can also cause more frequent periods so it is often used in conjunction with the oral contraceptive pill. Cyproterone may cause problems with menstrual periods if taken for a long period of time and, rarely, it may cause liver problems, although liver blood tests will be monitored whilst on this treatment.
Side-effects generally tend to resolve over time as the body adjusts to the medication, although a dose reduction or different formulation may be required if symptoms persist.
Long term, polycystic ovary syndrome can cause problems with fertility if a woman does not have a period for a prolonged time. It can also increase the risk of developing diabetes. If a woman goes for a long time without a period, the lining of the uterus can build up and some research studies suggest that this could potentially increase the risk of endometrial cancer. However, this risk is minimised by ensuring that periods occur at least once every three months. If a woman has any concerns about the longer-term implications of polycystic ovary syndrome, she should contact her GP.
Verity is a patient support group that may be able to provide advice and support to patients and families dealing with polycystic ovary syndrome.
Last reviewed: Nov 2021